You may have heard atrial fibrillation (AFib) described as an irregular heartbeat. However, that doesn’t fully capture how the condition behaves over time. AFib is a progressive heart rhythm disorder. This means that the longer someone has it, the worse it can get. While there is no cure for AFib, there are treatments to help restore a normal heart rhythm and reduce stroke risk.
AFib may start with short episodes that come and go. But over time, these episodes can happen more often and become harder to control. As AFib progresses, the risk of serious complications, such as stroke, heart failure, and premature death, increases.1 Protecting your long-term health starts with understanding how AFib may change over time and why ongoing management is so important.
How common is AFib?
AFib is the most common long-lasting heart rhythm problem in the world.1 In the United States, about 10.5 million Americans are living with AFib. As the population ages, this number is expected to grow.1
AFib happens when the heart’s electrical signals don’t work the right way. This causes the atria (upper chambers of the heart) to beat out of rhythm. The heart may also beat too fast. When this happens, the heart can’t pump blood as well as it should. Over time, this puts extra strain on the heart. AFib is associated with higher rates of stroke, heart failure, hospitalization, and death compared to people without the condition.2
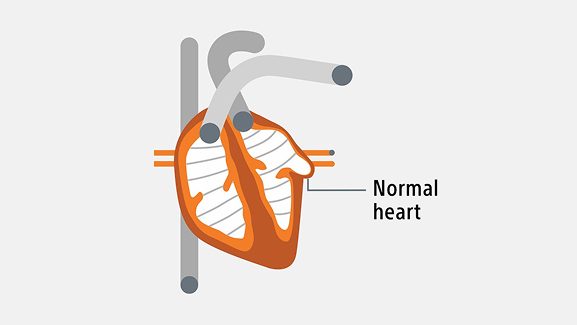
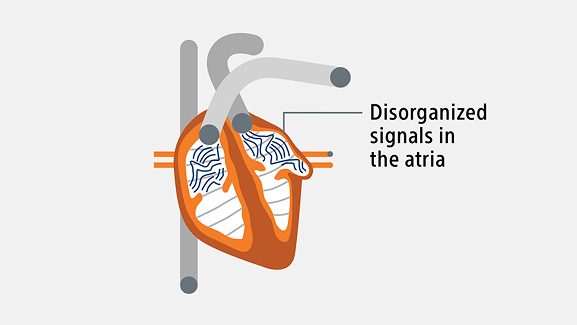
AFib is a progressive condition
AFib is a progressive disease, so if left untreated, it often gets worse over time. It can worsen faster when contributing risk factors such as high blood pressure, diabetes, obesity, or sleep apnea aren’t well controlled.2
Here’s how AFib can change over time:
- AFib often begins as “paroxysmal AFib.” This means episodes come and go, usually lasting less than seven days.3 Symptoms may include palpitations, fatigue, shortness of breath, or dizziness. However, some people experience few or no noticeable symptoms. Even at this stage, repeated AFib episodes can alter the heart’s electrical pathways and structure. This raises the likelihood that AFib will return.3
- Over time, paroxysmal AFib may progress to “persistent AFib.” In persistent AFib, episodes last longer than a week and may require medical intervention to restore normal heart rhythm.3
- Some individuals eventually develop long-standing persistent or “permanent AFib.” The more time the heart spends in AFib, the higher the risk of blood clots, stroke, heart failure, or other long-term effects.3
What are some of the long-term effects of AFib?
Stroke is one of the most serious risks of AFib.2 When the heart beats out of rhythm, blood can pool inside the heart. Over 90% of stroke-causing clots form in a small pouch called the left atrial appendage.4 Stagnant blood is more likely to form clots. If a clot travels from the heart to the brain, it can block blood flow, leading to an ischemic stroke.2

People with AFib are approximately five times more likely to have a stroke than those without it.5 AFib is also associated with heart failure, reduced quality of life, cognitive decline, and increased mortality.
How stroke risk increases over time
Stroke risk in AFib isn’t static. It increases with age and as AFib gets worse. Blood thinners can lower the risk, but they must be taken regularly and can increase the risk of bleeding. Because AFib is a lifelong condition, doctors need to check stroke and bleeding risk often and adjust treatment as health needs change.6
Learn more about the connection between AFib and stroke risk.
Maintaining your treatment plan vs. trying a different approach
Maintaining your current treatment plan might mean taking rate and rhythm medications or blood thinners long-term, as long as symptoms seem stable or stroke risk appears controlled. This approach works well for some. However, AFib can get worse without causing clear symptoms. An irregular heartbeat can still strain the heart and raise the risk of problems over time.
It’s important to talk to your doctor regularly about your treatment plan and how it works for your lifestyle. Active AFib management can look like regular follow-ups, reassessment of symptoms and stroke risk, and proactive conversations with a doctor about how treatment strategies should change as AFib changes and evolves.
Find out if you’re a candidate for the WATCHMAN Implant. Take the quiz
Stroke prevention is an important part of AFib treatment. Blood thinner medications are a common treatment to manage your stroke risk. However, these medications must be taken everyday to be effective. Additionally, blood thinner medications come with an increased risk of bleeding and other side effects.
The WATCHMAN Implant is an alternative to daily blood thinners to lower stroke risk for people with non-valvular AFib (NV-AFib). It’s placed during a safe, minimally-invasive, one-time procedure and never needs to be replaced.
There are risks associated with all medical procedures. Please talk with your doctor about the risks and benefits of the WATCHMAN Implant.
Commonly Asked Questions about AFib
What is a dangerous heart rate with AFib?
There's no one heart rate that’s dangerous for everyone. But when the heart beats too fast for long periods, it can weaken the heart. Over time, this increases the risk of heart failure.2
It’s important to recognize that AFib can appear “silent.” It can still raise the risk of stroke and heart failure, even without obvious symptoms.2 Routine monitoring and proactive care are critical, regardless of how stable symptoms may appear to be.
Is AFib life-threatening?
AFib is rarely life-threatening on its own. However, it significantly increases the risk of serious complications. People with AFib have a higher risk of stroke, heart failure, and hospitalization compared to those without the condition.2 Without active long-term management, these complications can become life-threatening over time.
Learn more about the long-term risks of AFib.
How can I slow AFib progression?
Treating AFib with cardiac ablation has been shown to slow its progression.7 It’s possible to get an ablation and a WATCHMAN Implant at once, treating AFib symptoms and stroke risk in one combined treatment.
Learn more about getting both procedures at the same time.
Can AFib cause death?
AFib is associated with an increased risk of death. This is largely due to complications such as stroke and heart failure. Studies show that people with AFib have a higher mortality risk than those without it.5 Follow-up care and active disease management can significantly mitigate these risks.
Can you live a normal life with AFib?
Many people with AFib are able to live active and fulfilling lives, especially with appropriate treatment and ongoing management. Medications, lifestyle changes, and medical procedures can help control symptoms and reduce complications. Outcomes are generally better for people who actively manage AFib and address related health conditions.
Taking an active role in AFib care
Living with AFib isn’t just about managing current symptoms — it’s about preserving long-term health for years to come. Recognizing AFib as a progressive condition can help you be more proactive in conversations with your doctor.
Already took the quiz? Return to your personalized experience.
References:
- Noubiap JJ, Tang JJ, Teraoka JT, et al. Minimum national prevalence of diagnosed atrial fibrillation inferred from California acute care facilities. J Am Coll Cardiol. 2024 Oct 15;84(16):1501-1508.
- FAQ About AFib. American Heart Association, Inc., 2023. Available at: www.heart.org/-/media/Files/Health-Topics/Atrial-Fibrillation/FAQ-About-AFib.pdf. Accessed June 10, 2024.
- Shah AJ, Hocini M, Komatsu Y, et al. The progressive nature of atrial fibrillation: a rationale for early restoration and maintenance of sinus rhythm. J Atr Fibrillation. 2013;6(2):849. doi:10.4022/jafib.849
- Left Atrial Appendage Closure (LAA). Cleveland Clinic. Available at: https://my.clevelandclinic.org/health/treatments/17167-left-atrial-appendage--closure. Accessed June 10, 2024.
- Ganjehei L, Massumi A, Razavi M, Abdi Rasekh. Stroke prevention in nonvalvular atrial fibrillation. Texas Heart Institute Journal. 2024;38(4):350.
- Joglar JA, Chung MK, Armbruster AL, et al. 2023 ACC/AHA/ACCP/HRS guideline for the diagnosis and management of atrial fibrillation: A report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2023;149(1). doi:10.1161/CIR.0000000000001193
- Kuck KH, Lebedev DS, Mikhaylov EN, et al. Catheter ablation or medical therapy to delay progression of atrial fibrillation: the randomized controlled atrial fibrillation progression trial (ATTEST). Europace. 2021;23(3):362–369.
All images are the property of Boston Scientific. All trademarks are the property of their respective owners.
Content on this web page is for Informational Purposes only and does not constitute medical advice and should not be used for medical diagnoses. Boston Scientific strongly recommends that you consult with your physician on all matters pertaining to your health or to address any clinical/medical questions.
Important Safety Information
The WATCHMAN FLX and WATCHMAN FLX Pro Devices are permanent implants designed to close the left atrial appendage in the heart in an effort to reduce the risk of stroke.
With all medical procedures there are risks associated with the implant procedure and the use of the device. The risks include, but are not limited to, accidental puncture of the heart causing fluid to collect around the heart possibly leading towards the need for an additional procedure, allergic reaction, anesthesia risks, altered mental status or confusion after procedure, arrhythmias (irregular heartbeats), bleeding or throat pain from the TEE (Trans Esophageal Echo) probe, chest pain/discomfort, congestive heart failure, renal failure, excessive bleeding, gastrointestinal bleeding, groin puncture bleed, bruising at the catheter insertion site, groin pain, anemia (reduced red blood cells requiring transfusion), hypotension, infection/pneumonia (example: in or around your heart or lungs), misplacement of the device, improper seal of the appendage or movement of device from appendage wall, clot formation on the device, blood clot or air bubbles in the lungs or other organs, stroke, transient ischemic attack (temporary stroke-like symptoms), cranial bleed (bleeding in or around your brain), thrombosis (blockage of a blood vessel or vein by a clot) and in rare cases death can occur.
Be sure to talk with your doctor so that you thoroughly understand all of the risks and benefits associated with the implantation of the device. SH-2109508-AA

