Did you know that people who have atrial fibrillation (AFib) have a five times higher risk of stroke than people with a regular heartbeat?1 A stroke can happen suddenly, but the risks build slowly and silently over time.2 If you’re living with AFib, it’s important to understand why strokes happen and how AFib increases your risk so you can take action to reduce your stroke risk.
What happens during a stroke?
A stroke happens when blood flow to a part of the brain is suddenly cut off. The brain relies on a constant supply of oxygen-rich blood delivered through arteries that carry blood from the heart. If one of the arteries becomes blocked or bursts, blood can’t reach the brain tissue it normally supplies. Without a steady supply of oxygen-rich blood, brain cells will begin to die. Even a short disruption in blood flow can cause lasting damage in the brain.2,3
You may hear doctors refer to a stroke with different names, such as a brain attack or a cerebrovascular accident (also known as the medical abbreviation CVA). These terms all mean the same thing.2,3
Stroke signs and symptoms
Depending on the part of the brain affected, a stroke can affect how you move, speak, or think. Common signs of a stroke include:2,3
- Face drooping
- Weakness in the arms
- Difficulty speaking
Other stroke symptoms may include sudden weakness or numbness on one side of the body, confusion, trouble seeing, difficulty walking, and severe headache. If you or a loved one experiences these symptoms, it’s important to act quickly. Every minute counts when someone is having a stroke.2,3
Stroke vs heart attack
A stroke and a heart attack both happen when blood flow is reduced or blocked.2-4 The key difference between a stroke and a heart attack is where the blockage occurs. During a stroke, blood flow to the brain is affected.2,3 During a heart attack, blood flow to the heart muscle is affected.4
The signs of a heart attack are also different from those of a stroke and may include:5
- Chest pain
- Pain in the arms, neck, back, shoulders, or stomach
- Shortness of breath
- Nausea
- Lightheadedness
Just like in a stroke, it’s important to seek medical attention right away if you experience any of these symptoms.5
What causes a stroke?
A stroke happens when blood flow to part of the brain is interrupted. There are different types of strokes, each with its own cause:2,3
- Ischemic stroke — When a blood clot blocks an artery supplying blood to the brain2,3,6
- Hemorrhagic stroke — When a blood vessel in the brain bursts and bleeds into the surrounding tissue2,3
- Transient ischemic attack (also known as the medical abbreviation TIA) — When blood flow to the brain is temporarily blocked by a clot that dissolves or moves on its own2,3,7
An ischemic stroke is the most common type of stroke. It accounts for about 87% of all strokes. During an ischemic stroke, a blood clot blocks one of the arteries providing blood to the brain. When the brain artery is blocked, it reduces blood flow (called ischemia).2,3,6
Blood clots that cause ischemic strokes can form in a blood vessel inside the brain or in another part of the body. When a blood clot forms in the heart and travels through the bloodstream to the brain, it can cause a type of ischemic stroke called a cerebral embolism (also known as an embolic stroke). AFib is the main cause of embolic strokes.2,3,6
Who is at risk for a stroke?
A stroke can affect anyone, but some people have a higher risk than others. Most people who have strokes are older than 55 years. Men are more likely to have a stroke than women. However, when women have a stroke, they’re more likely to die than men.3,8
AFib is one of the medical conditions that can increase your risk of stroke.9 Other health conditions that can also increase your risk of stroke include:3,8
- Overweight or obesity
- High blood pressure
- High cholesterol
- Diabetes
- Obstructive sleep apnea
- Heart disease, including heart failure and heart defects
- Recent or ongoing COVID-19 infection
- Frequent migraine headaches
There are some stroke risk factors that you can’t control, like your age, sex, and medical conditions.10 However, your lifestyle habits can also play a big role in your risk of stroke, such as:3,8
- Not getting enough physical activity
- Drinking alcohol
- Smoking or using other types of tobacco or vaping
- Using recreational drugs
Your doctor can help you understand which risk factors for stroke you may have.
Find out if you’re a candidate for the WATCHMAN Implant. Take the quiz
Why does AFib increase the risk of stroke?
In AFib, the atria (the upper chambers of the heart) beat irregularly. This irregular rhythm prevents the heart from efficiently pumping blood out of the heart with each beat.9
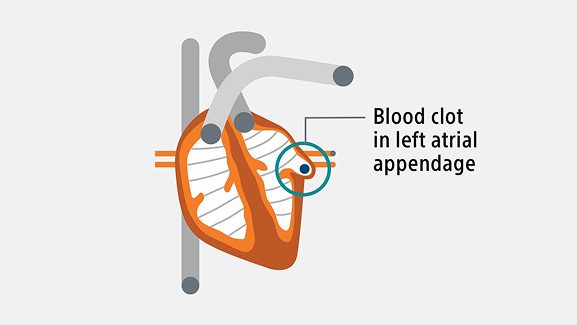
The blood left behind in the heart can begin to pool, making it easier for blood cells to stick together and form blood clots. Blood clots often form in a small pouch in the atria called the left atrial appendage (LAA). If a blood clot escapes from the LAA, it can travel to the brain and cause an embolic stroke. 9
A medical procedure to close off the LAA can reduce the risk of stroke.11 The WATCHMAN Implant is designed to close off the LAA to prevent blood clots that form here from entering the bloodstream.12,13
There are risks associated with all medical procedures. Please talk with your doctor about the risks and benefits of the WATCHMAN Implant.
How to reduce stroke risk with AFib?
Did you know that 1 out of 3 people with untreated AFib will have a stroke in their lifetime? 17 Reducing the risk of stroke is one the most important AFib treatments.14
If your doctor determines that your risk of stroke is high, they may recommend treatments to lower your risk. Blood thinner medications can help prevent the formation of blood clots. But blood thinners can come with side effects and other challenges, like an increased risk of bleeding.15 Learn more about how blood thinners work.
Some people with non-valvular AFib who need an alternative to blood thinners may be eligible for a permanent solution to close off the LAA, where most stroke-causing blood clots are formed.11,12 The WATCHMAN Implant is placed in a safe, minimally-invasive one-time procedure to permanently close the LAA. It reduces stroke risk for life – without the need for daily blood thinners.13 In a clinical trial, 96% of people were able to stop their blood thinner 45 days after getting the WATCHMAN Implant.13
Talk to your doctor about stroke protection
Someone in the United States has a stroke every 40 seconds.16 If you’re living with AFib, your risk of stroke is higher than those with a regular heart rhythm. It’s important to talk to your doctor about how to reduce your risk of stroke.
If you have non-valvular AFib and need an alternative to blood thinners to reduce your stroke risk, talk to your doctor about the WATCHMAN Implant.
Already took the quiz? Return to your personalized experience.
References:
- What is atrial fibrillation? American Heart Association website. Updated March 26, 2025. Accessed February 19, 2026. https://www.heart.org/en/health-topics/atrial-fibrillation/what-is-atrial-fibrillation-afib-or-af
- Explaining stroke. American Stroke Association website. Published 2020. Accessed February 19, 2026. https://www.stroke.org/en/-/media/Stroke-Files/Stroke-Resource-Center/Brochures/Explaining_Stroke_Brochure_2020.pdf?sc_lang=en
- Stroke. Cleveland Clinic website. Updated January 27, 2025. Accessed February 19, 2026. https://my.clevelandclinic.org/health/diseases/5601-stroke
- What is a heart attack? American Heart Association website. Updated December 10, 2024. Accessed February 19, 2026. https://www.heart.org/en/health-topics/heart-attack/about-heart-attacks
- Heart attack, stroke and cardiac arrest symptoms. American Heart Association website. Accessed February 19, 2026. https://www.heart.org/en/about-us/heart-attack-and-stroke-symptoms
- Ischemic stroke (clots). American Heart Association website. Accessed February 19, 2026. https://www.stroke.org/en/about-stroke/types-of-stroke/ischemic-stroke-clots
- Transient ischemic attack (TIA). American Heart Association website. Accessed February 19, 2026. https://www.stroke.org/en/about-stroke/types-of-stroke/tia-transient-ischemic-attack
- Stroke. Mayo Clinic website. Updated December 13, 2024. Accessed February 19, 2026. https://www.mayoclinic.org/diseases-conditions/stroke/symptoms-causes/syc-20350113
- Why atrial fibrillation matters. American Heart Association website. Updated March 26, 2025. Accessed February 19, 2026. https://www.heart.org/en/health-topics/atrial-fibrillation/why-atrial-fibrillation-af-or-afib-matters
- Preventing stroke. Centers for Disease Control and Prevention website. Updated May 15, 2024. Accessed February 19, 2026. https://www.cdc.gov/stroke/prevention/index.html
- Surgical procedures for atrial fibrillation. American Heart Association website. Updated May 6, 2025. Accessed February 19, 2026. https://www.heart.org/en/health-topics/atrial-fibrillation/treatment-and-prevention-of-atrial-fibrillation/surgical-procedures-for-atrial-fibrillation-afib-or-af
- Blackshear JL, Odell JA. Appendage obliteration to reduce stroke in cardiac surgical patients with atrial fibrillation. Ann Thorac Surg. 1996;61:755-759.
- Kar S., Doshi S., Sadhu A., et al. Primary Outcome Evaluation of the Next Generation LAAC device: Results from the PINNACLE FLX Trial. Circulation. 2021;143:1754–1762.
- How are atrial fibrillation treatment options determined? American Heart Association website. Updated May 6, 2025. Accessed February 19, 2026. https://www.heart.org/en/health-topics/atrial-fibrillation/treatment-and-prevention-of-atrial-fibrillation/treatment-options-of-atrial-fibrillation-afib-or-af
- Atrial fibrillation medications. American Heart Association website. Updated May 14, 2025. Accessed February 19, 2026. https://www.heart.org/en/health-topics/atrial-fibrillation/treatment-and-prevention-of-atrial-fibrillation/atrial-fibrillation-medications
- Stroke facts. Centers for Disease Control and Prevention website. Updated October 24, 2024. Accessed February 19, 2026. https://www.cdc.gov/stroke/data-research/facts-stats/index.html
- Blackshear JL, Odell JA. Appendage obliteration to reduce stroke in cardiac surgical patients with atrial fibrillation. Ann Thorac Surg. 1996;61:755-759.
All images are the property of Boston Scientific. All trademarks are the property of their respective owners.
Content on this web page is for Informational Purposes only and does not constitute medical advice and should not be used for medical diagnoses. Boston Scientific strongly recommends that you consult with your physician on all matters pertaining to your health or to address any clinical/medical questions.
Important Safety Information
The WATCHMAN FLX and WATCHMAN FLX Pro Devices are permanent implants designed to close the left atrial appendage in the heart in an effort to reduce the risk of stroke.
With all medical procedures there are risks associated with the implant procedure and the use of the device. The risks include, but are not limited to, accidental puncture of the heart causing fluid to collect around the heart possibly leading towards the need for an additional procedure, allergic reaction, anesthesia risks, altered mental status or confusion after procedure, arrhythmias (irregular heartbeats), bleeding or throat pain from the TEE (Trans Esophageal Echo) probe, chest pain/discomfort, congestive heart failure, renal failure, excessive bleeding, gastrointestinal bleeding, groin puncture bleed, bruising at the catheter insertion site, groin pain, anemia (reduced red blood cells requiring transfusion), hypotension, infection/pneumonia (example: in or around your heart or lungs), misplacement of the device, improper seal of the appendage or movement of device from appendage wall, clot formation on the device, blood clot or air bubbles in the lungs or other organs, stroke, transient ischemic attack (temporary stroke-like symptoms), cranial bleed (bleeding in or around your brain), thrombosis (blockage of a blood vessel or vein by a clot) and in rare cases death can occur.
Be sure to talk with your doctor so that you thoroughly understand all of the risks and benefits associated with the implantation of the device. SH-2109508-AA

